Dr Jinan Harith Darwish is a paediatric allergy specialist and clinical immunology fellow at the King Faisal Specialist Hospital & Research Center. Each month she answers your parenting questions.
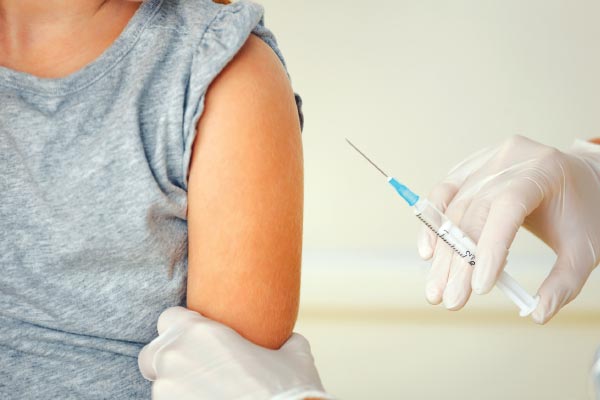
To Vaccinate or Not TO Vaccinate?
I’ve read a lot about the human papillomavirus vaccine (HPV) for young girls. My doctor is advising it but there seems to be some controversy surrounding it. What are your thoughts please doctor?
HPV has long haunted the human race; nearly all sexually active adults carry some of HPVs’ 170 strains. And while many of these are harmless, amid the multitude mutants there are those with effects that are anything but benign: subtypes 6 and 11 can lead to genital warts; subtypes 16 and 18, amongst others, can lead to cervical, vulvar, vaginal, penile, anal and oral cancers. Type 16 together with type 18 is responsible for 70 per cent of the cases of cervical cancer in Europe; and types 6 and 11 together are responsible for around 90 per cent of cases of genital warts. This is not some mere hypothetical risk – over 90 per cent of cervical cancers are caused by HPV, a cancer which claimed the lives of 270,000 women worldwide in 2012 alone.
Cervical cancer is the most common cancer among women aged 15 to 34. Unlike the majority of cancers, it is mainly a disease of the young, with 62 per cent of cases occurring in women who are under 50. The American Cancer Society’s estimates for cervical cancer in the United States for 2016 are:
About 12,990 new cases of invasive cervical cancer will be diagnosed.
About 4,120 women will die from cervical cancer.
The vaccine currently used in the UK is called Gardasil. It was chosen over an alternative called Cervarix because it gives wider protection. In clinical trials, Gardasil was over 99 per cent effective at averting cancer caused by HPV types 16 or 18 in young women, and it is expected that vaccination will reduce the number of cases of the most common kind of cervical cancer by at least 70 per cent. However, it is important that girls who are vaccinated continue to take up the offer of cervical smear testing later in life, so that other kinds of cervical cancer can be picked up.
HPV world-wide vaccine programmes are currently being appraised. Evidence from these shows falling numbers of young people with pre-cancerous cells, and protection from the HPV vaccine is expected to be long-term.
The Public Health England 2015 report shows a significant fall in HPV infections in young women since the vaccine was introduced. In 2010-13, HPV types 16 and 18 were 66 per cent less common in sexually active young women aged 16 to 18 than they were in 2008. These early findings support the view that the HPV vaccination programme will have an impact on the numbers of cases of cervical cancer in future. Before September 2014, girls in the UK received three doses of the HPV vaccine. However, from September 2014 the number of doses was reduced from three to two for those who first receive the vaccine aged 12 to 13.
This was because research has demonstrated that two doses of the vaccine give a level of protection that is just as good and lasts just as long as three doses, as long as girls are aged 12 to 13 at first dose. For those who start the vaccination course over the age of 13, it is recommended that they continue to receive the three doses.
In Australia, data from sexual health clinics illustrate that cases of genital warts in younger women have fallen since vaccination was initiated. In 2007, the year HPV vaccination started, over 11 per cent of women under 21 were diagnosed with genital warts at their first visit to a clinic. By 2014 this number had fallen to just over one per cent. There was also a decline in cases among 21 to 30-year-old women; some of these would have been vaccinated against HPV. In the over 30 age group, who did not receive HPV vaccination, there was no change between 2007 and 2014.
Sadly, scaremongering anecdotes without scientific evidence all too often masquerade unchallenged as public interest stories, and the Gardasil controversy is no exception. The question is are they anti-cancer or are they anti-sex? A major apprehension appears to be that without the trepidation of genital warts or cervical cancer, young individuals will become more promiscuous, and that the HPV vaccine hence, in effect, promotes behaviour deemed immoral. We cannot afford to allow squeamishness on the subject of sex to dictate health policy, nor should we permit myths to blur our judgement. The lives of countless young women and men count on us being guided by evidence rather than rhetoric.
The second category of opposition is rooted in safety fears. Like all clinical compounds, Gardasil has been extensively tested for years, constantly monitored for potential adverse effects. By all measures it has been found to be a safe and effective intervention. The complication rate is low, with the most frequent reactions being irritation at the site of injection, and fainting post-injection – precisely the minor temporary reactions seen with any shot.
The case for the safety of the HPV vaccine is supported by myriads of clinical substantiation and years of data, whereas the opposing side is comprised of anecdotes, emotive petition and effortlessly exposed allegations. Despite all the sound and fury, the unassailable nitty-gritty of the matter is that the HPV vaccine has the potential to save lives.
Sport Crazy
 My son is obsessed with sport. He seems healthy and fit but does seem to get a lot of injuries and I struggle to get him to eat enough. How do I make sure he’s not missing out on essential dietary requirements?
My son is obsessed with sport. He seems healthy and fit but does seem to get a lot of injuries and I struggle to get him to eat enough. How do I make sure he’s not missing out on essential dietary requirements?
Too frequently we hear about the millions of children and adolescents who are sedentary, overweight and obese. The amount of physical activity recommended for kids aged six to 17 is at least one hour per day of indoor or outdoor sport all year round.
F The experts’ thinking about the needs of active youths and how hormones may influence child athletes is changing. While not everyone agrees with the specifics, there’s one common refrain: Children are not small adults. Their rapid growth and increase in muscle mass changes their nutrient and fluid needs in unique ways.
The distribution of macronutrients recommended for active children and child athletes is the same as for less active peers.
Protein aids muscle recovery when consumed after exercise and should account for 10 to 15 per cent of calories. Recommendations for total protein intake are 0.95g/kg/day for kids aged four to 13 and 0.85g/kg/day for adolescents aged 14 to 18.
Carbohydrate is the most important source of energy for an active child or adolescent and should represent 55 per cent of calories (more on heavy training days), about five to eight grams per kilogram of body weight.
Fat should account for 25 to 30 per cent of total calories. Emphasise the wholesome fat that’s found in avocados, tuna, canola oil, soy and nuts.
Fluid intake should be overseen and monitored during and after physical activity. This should result in an hourly fluid intake of 13ml/kg. Fluid replacement post-exercise should include about 4ml/kg for each hour of activity. More is needed for children who sweat heavily.
Delayed Development
 My daughter will be 14 in July but hasn’t yet started her periods. Is this normal or should I take her to the doctor?
My daughter will be 14 in July but hasn’t yet started her periods. Is this normal or should I take her to the doctor?
Puberty starts when the pituitary gland begins to produce two hormones, luteinising hormone (LH) and follicle-stimulating hormone (FSH), which cause the ovaries to enlarge and begin producing oestrogens. The growth spurt starts shortly after breasts begin to develop, and the first menstrual cycle begins about two to three years later. A girl who has not started to have breast development by the age of 13 is considered to be delayed.
Some girls with delayed puberty are simply late maturers, but once they start, puberty will progress normally. This is called constitutional delayed puberty. So it is likely to occur if the mother started her periods after age 14 (the average is about 12 and a half) or if the father was a ‘late bloomer’.
Decreased body fat is a major cause of pubertal delay in girls. It can be seen in girls who are very athletic.
If these aren’t the case, I suggest you visit a paediatric endocrinologist who will provide you with expert opinion.
If you have a question for Dr Jinan, please email [email protected]