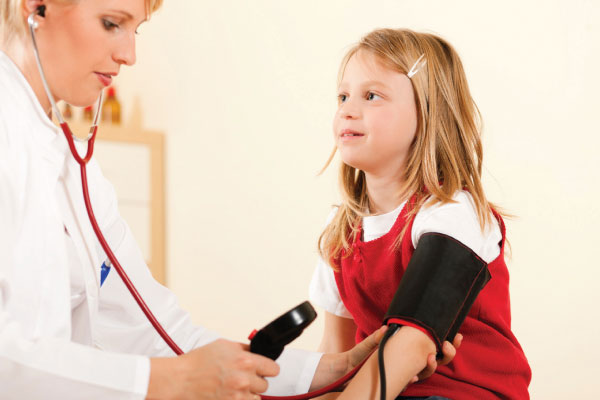
Gone are the days when hypertension was stereotypically an adult disease. A growing number of school students are being diagnosed with high blood pressure.
Blood pressure is defined as the amount of pressure exerted on the walls of the arteries as the blood travels through them. Prehypertension is defined as blood pressure in at least the 90th percentile, but less than the 95th percentile, or a measurement of 120/80mm Hg or greater.
Hypertension in children is defined as raised blood pressure above the 95th percentile for age, gender and height on three or more separate occasions. In individuals three to 18 years of age, the prevalence of prehypertension is 3.4 percent and the prevalence of hypertension is 3.6 percent. If blood pressure is greater than the 90th percentile, the measurement should be repeated during the same office visit to confirm validity.
Hypertensive children are likely to be asymptomatic in initial stages and thus blood pressure measurement should be a routine practice at any clinical contact. The National High Blood Pressure Education Program (NHBPEP) recommends measuring blood pressure at every office visit beginning at three years of age. Hypertensive children should be recognised promptly and suitably treating treatable any underlying cause to avoid end organ damage.
Many automatic blood pressure machines are unreliable in children, particularly when the blood pressure is outside the normal range. Repeated measurement is necessary to decide if the systolic blood pressure is rightly elevated and to exclude reactive rises. White coat hypertension is recognised in children where reactive raised blood pressure is seen in a nervous child.
A study published in the American Family Physician Journal found that secondary hypertension in children is far more common than essential hypertension. Secondary hypertension is high blood pressure as a result of another underlying condition or disease.
Before commencing a child on anti-hypertensive treatment it is crucial that any secondary factors, such as medications and pain, be removed.
Regular, sustained physical activity is most effective in lowering blood pressure, and the NHBPEP recommends 30 to 60 minutes of moderate aerobic physical activity on most days and less than two hours of sedentary activity per day. There is a lack of evidence that dietary interventions can significantly decrease blood pressure in children.
Nevertheless, experts maintain that children with hypertension may benefit from consuming a diet high in fresh fruits and vegetables, fibre, and non-fat dairy products, in addition to reducing sodium intake. One study found that the DASH (Dietary Approaches to Stop Hypertension) diet significantly lowered blood pressure
in adolescents compared with standard dietary counselling.
The aim is to bring the blood pressure between the 50th and 75th percentile for height and gender. Tailored treatment depends on the cause, duration and severity of the hypertension. If a child is suspected to have hypertension of unknown or long duration it must be lowered slowly.
Emergency Cases
Early diagnosis, aggressive but careful management depending on specific causes, and long-term follow-up will help in decreasing some of the burden. Hypertensive emergency in children is an indication for admission to intensive care unit for close monitoring and prompt initiation of appropriate intravenous antihypertensive therapy depending upon the cause. The goal is to lower the systolic blood pressure by one-third every 24 hours to avoid rapid decrease of blood pressure, which can result in a stroke from under perfusion of the brain. Once the acute rise in blood pressure settles oral anti-hypertensives could be instigated.