Whether you are in the prime of life, or older and wiser, it’s important to safeguard your skeletal structure from going brittle on you. Behnaz Sanjana finds osteoporosis doesn’t tickle the funny bone.
Dr Aleksandar Dimic, rheumatology and internal medicine consultant at Bahrain Specialist Hospital, explains the debilitating disease succinctly: “Osteoporosis is porous bones.” He goes on to say that when bones get rarified due to this condition, they fracture easily.
There are different types of osteoporosis, but the most common is age-related and afflicts women – post-menopausal osteoporosis. The onset of menopause sees an abrupt fall in oestrogen levels, which causes osteoporosis. Younger women who suffer amenorrhea or have undergone a hysterectomy also face the possibility of developing osteoporosis due to low levels of oestrogen. Malabsorption of calcium due to gastro intestinal issues is also a potential cause. “There is tight correlation between osteoporosis and levels of oestrogen, no matter the age,” says Dr Dimic.
He goes on to explain that there are two kinds of bones – the cortical bone and the trabecular bone – the latter being more prone to osteoporosis because it is seven to 10 times more metabolically active than the cortical bone. “The majority of trabecular bone is found in the vertebrae and a part of the femur called the femoral neck. Thus, the most frequent sites of fractures due to osteoporosis are in the vertebrae and the femur,” he says.
 Dr Dimic sees a lot of patients, primarily women, who walk into his clinic with this bone condition. He says, “The epidemiology of osteoporosis says that every second woman after the age of 50 will have osteoporosis. And from those women, every second or third woman will suffer from fractures.”
Dr Dimic sees a lot of patients, primarily women, who walk into his clinic with this bone condition. He says, “The epidemiology of osteoporosis says that every second woman after the age of 50 will have osteoporosis. And from those women, every second or third woman will suffer from fractures.”
Men can get osteoporosis too, but it is rarer than in women. Men can get it in their late sixties or seventies, due to lack of the hormone testosterone.
What’s unnerving about the osteoporosis story is that there are no definite symptoms, or there may be seemingly ambiguous ones, like back pain. The very first manifestation of the condition is a fracture.
It is being called a pandemic disease, because it is estimated today that around 200 million women in the world have osteoporosis. “Fractures caused due to it call for a major operation and can be life threatening. The rate of mortality is 20 per cent in the first year. Forty to 50 per cent of women who have suffered a femoral neck fracture will suffer some disability throughout life. They may not be able to cope with the demands of working life, or even everyday life easily,” warns the doctor.
In light of the terrible effects this disease can have, Dr Dimic cannot stress enough the importance for women over the age of 50 in reporting for the DXA test, taking into account their risk factors. “Risk factors are early menopause, in your forties or late thirties, a very thin body or a high caffeine intake [because caffeine absorbs a lot of the body’s calcium]. Other major concerns are smoking, high intake of alcohol and lack of physical exercise, which increases bone mineral density. Heredity is also a major factor determining whether a woman will suffer osteoporosis,” he says.
Regular check-ups are imperative – once every year if osteopenia is diagnosed and once every two years if you have normal results. The outcome of treatment for osteoporosis should also be assessed every year. Calcium and vitamin D supplements and a healthy lifestyle including weight-bearing exercise are the best course to prevent osteopenia from turning into full-blown osteoporosis.
If you’re a way off from turning 50, now is the time to take preventive measures against this disorder. Dr Dimic explains why: “Women achieve peak bone mass around their 20s. Adequate vitamin D through sunshine, calcium and physical activity in the adolescent period can achieve peak bone mineral density. If this is achieved, it’s less likely for osteoporosis to set in later in life. Bone mineral density peaks in adolescence and reaches a plateau till the age of 50, after which there is an abrupt dip in levels. If you have an appropriate peak, it is less likely to go under the minus 2.5 levels.”
He advocates that there is no need for calcium supplements if you stock up well on calcium naturally available in dairy products, fish and vegetables. He does mention though, that women must keep track of and be aware of their calcium intake as well. “Women need one gram of calcium, and one to 1.5 grams of calcium every day after the 50-year mark. Drinking 250 mililitres of milk is 100 to 200 miligrams of calcium, 100 grams of cheese is 200 to 300 miligrams of calcium. If you eat less dairy products, then take a supplement.”
 Know the Score
Know the Score
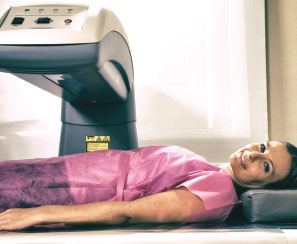
Osteoporosis is diagnosed by assessing one’s bone mineral density. A bone mineral density (BMD) test measures how much calcium and other types of minerals are in a specific area of your bone, the result of which is a T score. “A score of up to minus one indicates normal bone density. A T score lower than minus 2.5 indicates osteoporosis, and needs to be treated with bisphosphonates, a class of drugs that prevent the loss of bone mass. If this low score is accompanied with a fracture, then it is termed as severe osteoporosis,” he explains.
A T score below minus one, but higher than minus 2.5 is osteopenia. It indicates low bone density, and is a precursor to Osteoporosis. “If left untreated, it will develop into osteoporosis in the future. Proper treatment can halt it in its tracks,” states Dr Dimic.
BMD is measured by a Dexa-Scan (dual-energy X-ray absorptiometry or DXA) which uses a low energy X-ray to evaluate bone density in the hip and/or spine.
 Spill the Milk
Spill the Milk
If you’re not keen on dairy foods but don’t want to take a supplement, there are plenty of other natural sources of calcium such as kale, figs, oranges, white beans, okra, tinned salmon, almonds, black eyed peas, sesame seeds and tofu.